| Table of Contents |  |
|
Original Article
| ||||||
| Does seeking knowledge of depression make a difference? A randomized study to examine the efficacy of psychoeducational intervention with patients suffering from non-psychotic depression | ||||||
| Adel Gabriel | ||||||
|
FRCPC, MSc, DPIP, DPM, DTM & H, Consultant & Clinical Associate Professor, Departments of Psychiatry and Community Health Sciences, University of Calgary.
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
[Print This Article]
[Similar article in Pumed] [Similar article in Google Scholar] |
| How to cite this article |
| Gabriel A. Does seeking knowledge of depression make a difference? A randomized study to examine the efficacy of psychoeducational intervention with patients suffering from non-psychotic depression. Edorium J Psychiatry 2015;1:1–10. |
|
Abstract
|
|
Aims:
The primary objective of the study is to assess the efficacy of a systematic patient-centered psychoeducation program on knowledge seeking of depression and on the clinical outcomes, in patients with non-psychotic major depressive disorder.
Method: 52 consenting patients with confirmed diagnosis of major depression were randomly assigned to a group (n = 32) who received systematized psychoeducation for depression, and to a waiting group (n = 20) who received standard care. The intervention group received systematic education consisting of (i) Reading material, "depression manual", and (ii) individual or groups educational sessions. The primary clinical outcome measures included the clinician rated quick inventory of depressive symptomatology (QIDS-C) and the self-rated quick inventory of depressive symptomatology (QIDS-SR). Patients in both groups completed QIDS-SR, and the knowledge seeking behavior instrument (KSI), at baseline, at 4th, 8th and 12th weeks. Results: At 12th week, there was significant (p< 0.01) reduction in the (QIDS-CR) and the (QIDS-SR) scores in both the intervention and waiting group patients. However, there were significant differences between the two groups, with the superiority for the intervention group in reduction of depressive symptoms. The number of hours spent in knowledge seeking as measured by the (KSI), correlated negatively with the scores of QIDS-SR, and QIDS-CR. Conclusion: Systematized education may lead to significant reduction in clinical symptomatology, and to improved knowledge seeking behavior. | |
|
Keywords:
Clinical outcomes, Depression, Psychoeducational methods, Seeking knowledge
| |
|
Introduction
| ||||||
|
Depression is a major epidemiological concern, not only because of its high prevalence in the community but also because of its association with elevated risks of hospitalization and suicide. Over the last two decades, methods have been available to make valid and reliable assessment of the extent of depression in the community [1]. The relationship between depression literacy per se and behavior change, such as help-seeking, was examined in a number of studies. There is evidence in literature to support that patient knowledge of and attitudes towards depression and its treatment influence the choice of treatment modalities, especially antidepressant medication. For example, in a number of studies, the most frequently endorsed reasons for depressed individuals delaying or not seeking professional help or treatment was related to the lack of knowledge about mental illness and available treatments [2] [3] [4]. Does psychoeducation using multiple educational methods lead to favorable clinical outcome? Also, in another study, depressed primary care patients were randomized in a clinical trial exploring the effects of psychoeducation, to assess the outcomes of utilizing three educational methods. Patients (n = 108) assigned to this method of treatment received a package of educational materials at the time of the baseline interview. These materials included two brief interactive booklets (medication booklet, behavioral health booklet) and a short video. Intervention patients were interviewed on the telephone one week after they received the package of educational materials. Approximately, three-quarters of the subjects reported that they read or viewed all of the educational products. The majority rated the products as somewhat to significantly helpful, as follows: medication booklet 81%, behavioral health booklet 82% and video 69% [6]. Other studies found significantly better medication adherence and improved clinical outcomes for those patients with major depression who received a primary care intervention that included the educational products. It was also demonstrated in a number of studies that patients who received systematic patient education and ongoing monitoring of medication adherence and depressive symptoms had high rates of use of maintenance pharmacotherapy when compared to standard care patients [7] [8] [9] [10] [11] [12]. In a popular study for treating patients with depression, there was an increase in the remission rates from 3–12 months among outpatients who were treated with a medication algorithm and patient/family education package. This package included a comprehensive patient education manual, a video, a guide for patients and families, a medication fact sheet, and regular interactive educational sessions and discussions with a therapist over a 12-week period [12]. The majority of the intervention studies used multiple approaches, and educational approaches were parts of few interventions such as counseling and psychotherapy, all of which had the same objectives of improving adherence to antidepressants to reduce relapses through enhancing the learning experiences and using educational packages such as interactive booklets, self-help materials, and short videos, and telephone counseling [13]. For example, in a large psychoeducational intervention study, patients with recurrent major depression (n = 386) were randomized to a relapse prevention program. Patients in the intervention group received two primary-care visits with a depression specialist and three telephone visits over a one-year period, aimed at enhancing adherence to antidepressant medication and recognition of prodromal symptoms, and their symptoms were monitored. Those in the intervention group showed significantly greater adherence to adequate dosage of antidepressant medication for 90 days or more within the first and second six-month periods and were significantly more likely to refill medication prescriptions during the 12-month follow-up compared with usual care controls. Intervention patients had significantly fewer depressive symptoms, but not fewer episodes of relapse/recurrence over the 12-month follow-up period [9]. Also, in a collaborative care-management program for the elderly, patients (n = 1801) were randomized into an intervention group and a usual care group for up to 12 months, with the intervention group being offered education, antidepressant management or brief psychotherapy, and problem-solving for depression. Authors reported that intervention patients had a 50% or greater reduction in depressive symptoms from baseline, less functional impairment, and better quality of life compared with 19% of usual care participants at 3rd, 6th, and 12th months [10]. Psychoeducational methods in depression The lack of strong evidence for reliability and content validity and the quality of the presented material were critically examined in literature for being too medically orients and for being poorly patient-centered. For example in one study, views were expressed from 30 members of a self-help group of patients with depression, in which most members had concerns about the leaflets focusing on depression stigma and poor sense of self. We suggested that leaflets should reflect on patient's experience of the condition [21]. Hence, was the decision for the development of the KSI, with acceptable reliability and demonstrated validity [22]. To the best of our knowledge, there is no published study that examined the efficacy of seeking knowledge, among depressed patients utilizing a reliable instrument to measure knowledge seeking behavior, on depressive symptomatology. The objectives of this study was set to test the efficacy of psychoeducation on improving the knowledge seeking behavior among patients with non-psychotic depression, and to examine the relationship between the extent of time spent in seeking depression knowledge, and changes in depression symptomatology. | ||||||
|
Materials and Methods
| ||||||
|
Design Participants Inclusion / exclusion Criteria | ||||||
|
Psychoeducational Intervention
| ||||||
|
Randomization and procedure Components of educational methods
The standard care group (waiting group), were followed by the research psychiatrist, received standard care for major depression, including antidepressants, and counseling as necessary. These patients had the choice of receiving the educational program, should they wish, after the trial has been completed (12 weeks). All patients completed at least six visits with the research psychiatrist during the trial period. Patients in both groups (psychotherapeutic intervention or waiting) were treated by SSRIs or SNRIs antidepressants, and were followed by their psychiatrist once every four weeks, to review antidepressant treatments and addressing their educational and treatment concerns. Patients randomized to the educational intervention group were required for the purpose of this study, to complete at least attendance of four group sessions, or six individual educational sessions with the research psychiatrist. | ||||||
|
Evaluation and Assessments of Clinical Outcome
| ||||||
|
The primary efficacy assessments The Knowledge Seeking Instrument Data Analysis | ||||||
|
Results | ||||||
|
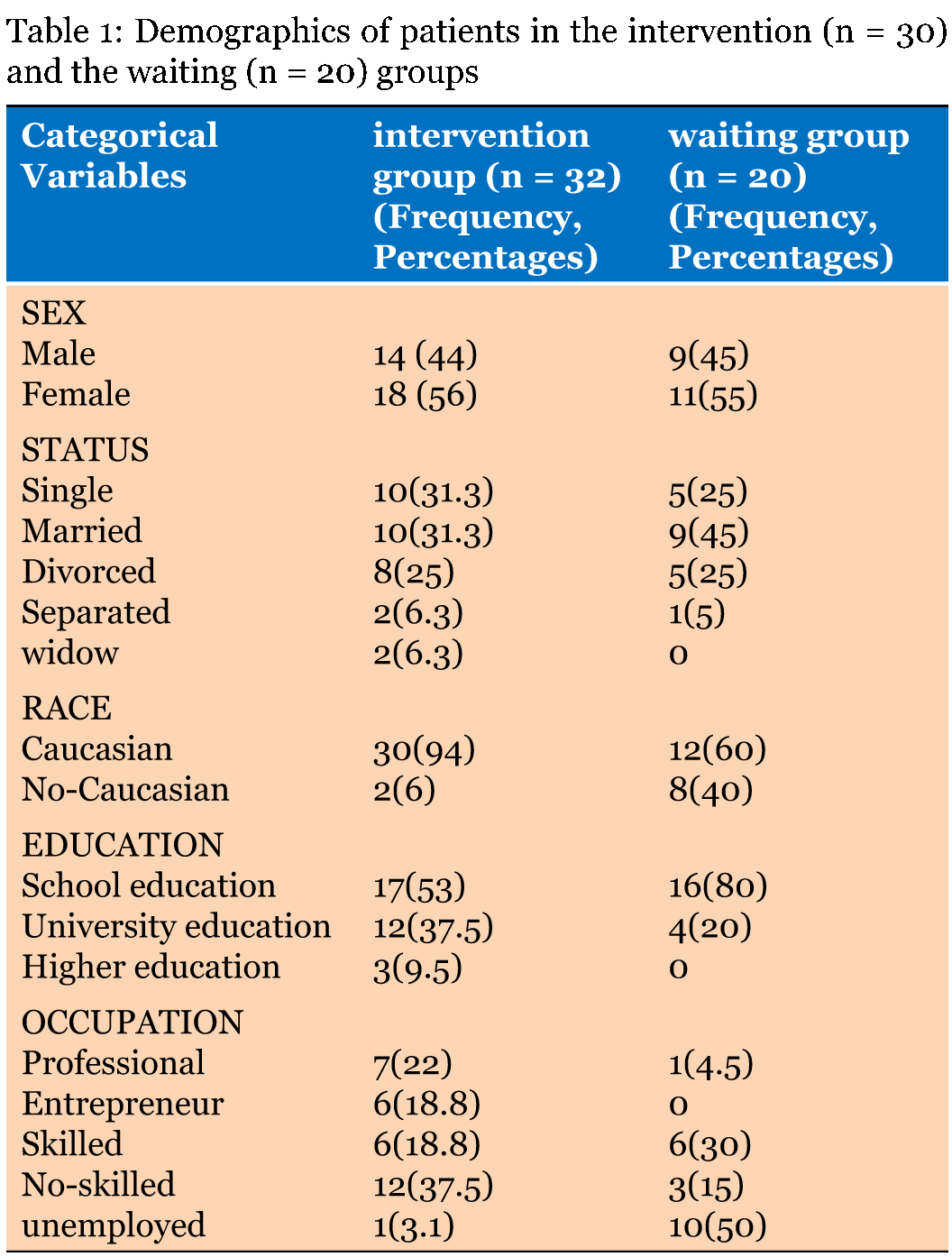
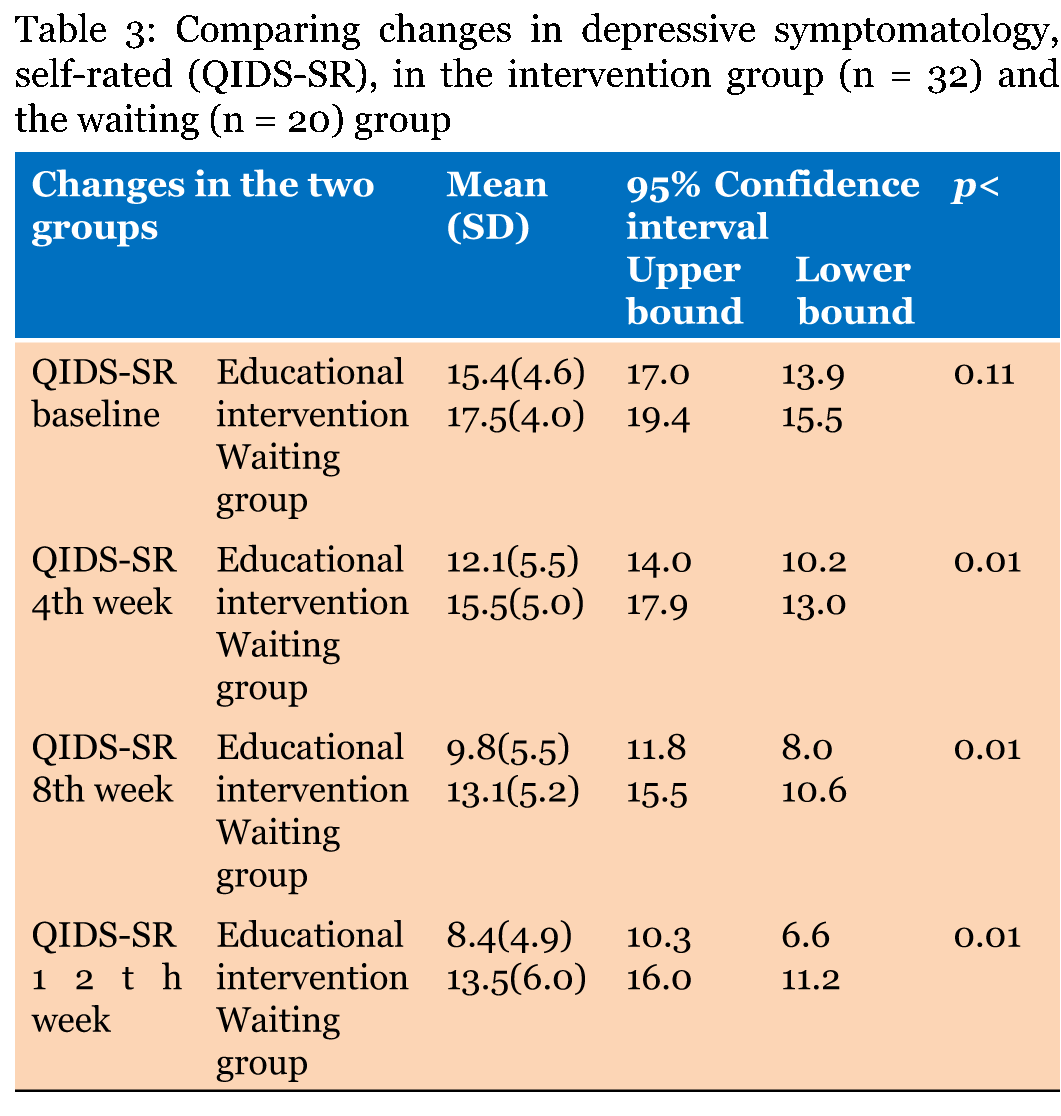
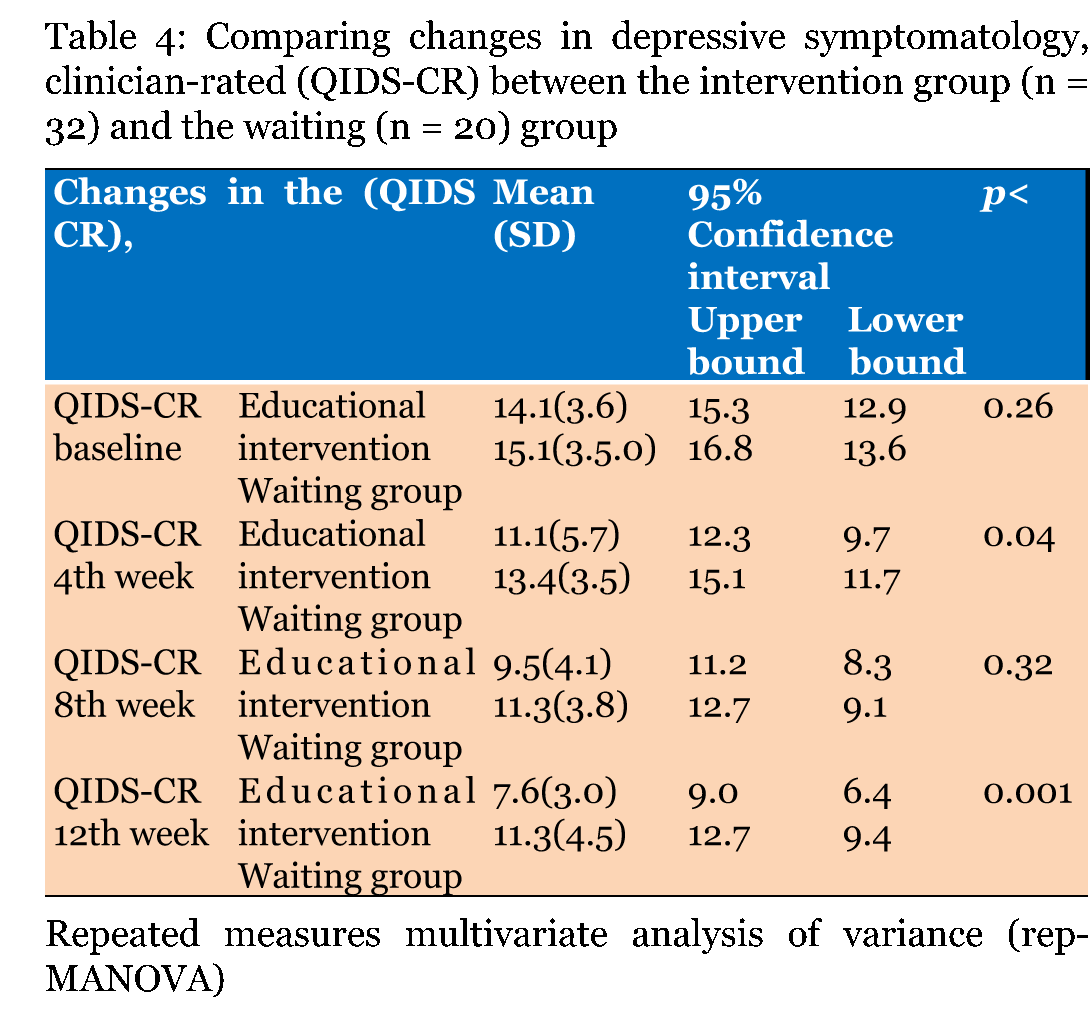
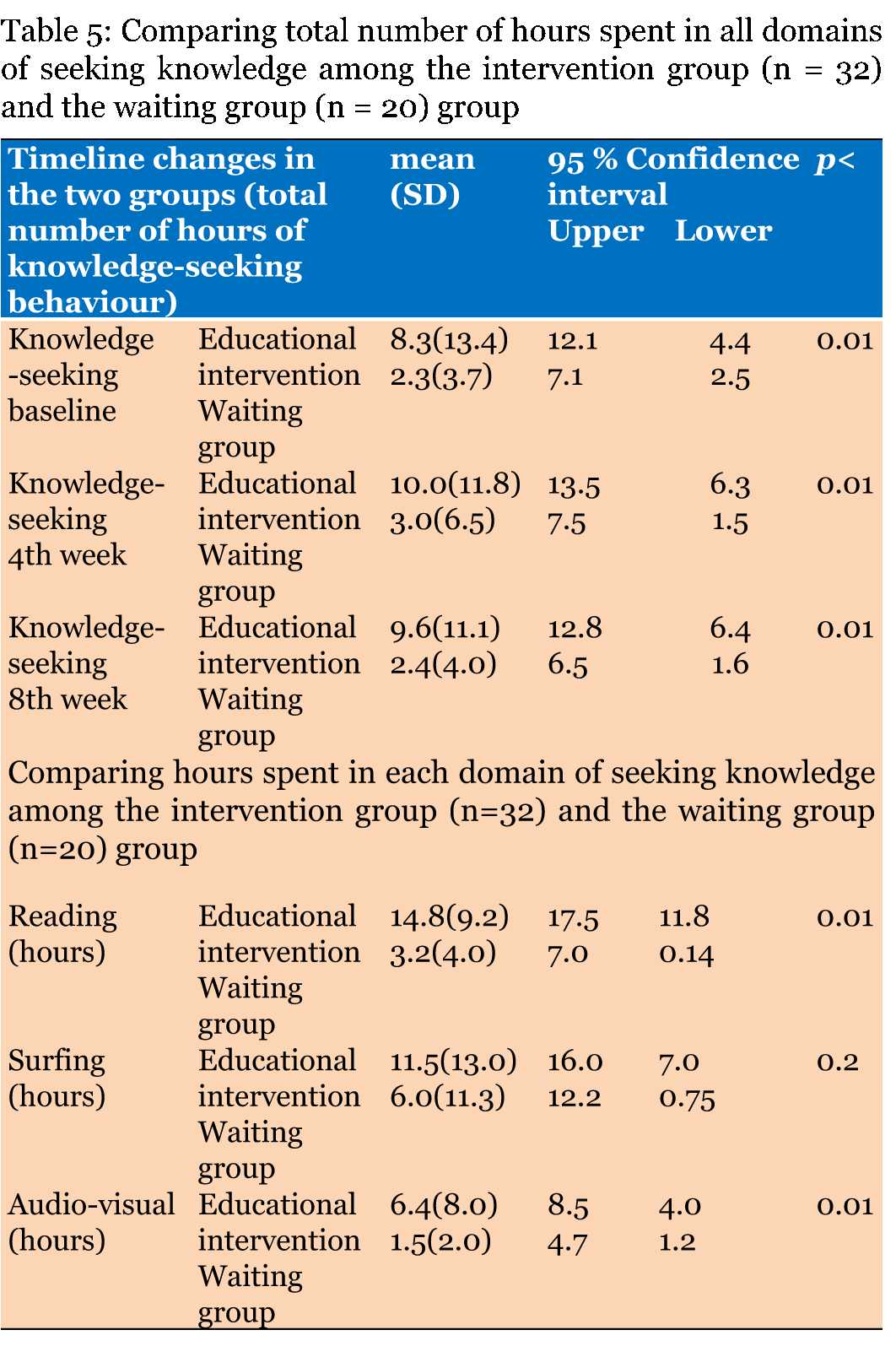
Completed the 12th-week study (n = 32) patients, randomized to the intervention an groups and (n = 20) randomized to the waiting group. Table 1 gives the demographic variables for both groups. Fifteen patients completed group sessions with a clinical educational psychologist, and seventeen patients attended individual educational sessions with a psychiatrist. All patients attended their psychiatrists to address standard treatments and the administration of antidepressants. The internal consistency reliability of knowledge seeking (KSI) instrument was reviewed in this study. The Cronbach's alpha measure was 0.72 at baseline (Table 1) and (Table 2). Depressive symptomatology QIDS-CR and QIDS-SR Paired sample t-test was employed to examine and compare changes in the mean depressive symptomatology QIDS-SR, and QIDS-CR at 12th week, from baseline, in the two groups. There was significant reduction (p<0.001) in depressive symptomatology measures in both groups. The general linear model, multivariate analysis of variance was utilized to examine the difference in depressive symptomatology changes between the intervention and waiting groups. Table 3 and Table 4 compare changes describe the changes in scores of QIDS-SR, and QIDS-CR in both groups (the educational intervention and the waiting). A close inspection of Table 3, there is significant difference (p<0.1) between the two groups, in QIDS-SR scores, the primary outcome measure at 4th, 8th and 12th weeks. Also there is significant differences in QIDS-CR scores between the two groups, at 4th week (p<0.04), and at 12th week (p<0.01) of treatment. There were no significant differences between the two groups in age, duration of depression, and length of the most recent episode or the number of times they received standard psychoeducational visits with a psychiatrist. There were significant positive correlations between QIDS-SR and QIDS-CR scores at baseline, at 4th, 8th, and 12th weeks r = 0.6, 0.66, 0.76, 0.75, respectively with p<0.001. Knowledge seeking behavior Table 5 gives the differences between the intervention and waiting groups in utilizing the three educational methods. A close inspection of this table, there is significant differences (p<0.1) between the overall time spent in utilizing one or more of the educational methods, and there were significant differences (p<0.1) between the two groups in the mean time spent on reading or in using audiovisual material. There were no significant differences between the two groups in age, duration of depression, and length of the most recent episode or the number of times they received standard psychoeducational visits with a psychiatrist. The relationship between knowledge seeking and changes in depressive symptomatology A close inspection of Table 6, there is significant inverse relationships, (negative correlations) between the severity of depressive symptomatology QIDS-SR, and QIDS-CR over time, and the overall number of hours spent learning about depression and its treatment, suggesting that individuals who sought more knowledge about depression and its treatments were likely to present with less symptoms on the QIDS-SR, and QIDS-CR. | ||||||
| ||||||
| ||||||
| ||||||
| ||||||
| ||||||
|
| ||||||
| ||||||
|
Discussion
| ||||||
|
This was a randomized single blinded study to examine the clinical outcomes of systematized depression education in patients with non-psychotic depression. The extent of knowledge seeking as measured by the number of hours spent in learning about depression was measured by an instrument with an established acceptable reliability from a previous study, and with evidence for validity [22]. Patients in the intervention group received a systematic education about depression utilizing multiple educational methods, utilizing reading material, were involved in discussions, and reflection on their experience either in groups or on an individual basis. The waiting group patients, although did not receive such systematic education, some were motivated and managed to learn about depression on their own from different educational sources. The intervention group have significantly utilized more time in learning and seeking depression knowledge, and were significantly less symptomatic than the waiting group. The rationale behind using multiple educational methods is justified by the fact that individuals have different preferences for learning referred to as learning styles [27]. The behavioral (i.e., psychomotor) aspect represents an essential learning domain of the learning theory [28]. In this study, I selected the behavior of patient knowledge seeking of depression and its treatment, as the psychomotor educational domain. Assessing and measuring the behavioral aspects of knowledge seeking among patients is considered as an integral part of assessing depression literacy, because it reflects, not only the motivation to seek different treatment modalities, but also that they have internalized and acted on their desire to learn by seeking knowledge about depression and its treatment. In this study, I utilized the first developed instrument to measure knowledge seeking, with established acceptable reliability, and with evidence for validity [22], in order to examine the relationship between KSI scores and depressive symptomatology measures QIDS-SR, and QIDS-CR in more depth. There are number of studies which examined the relationship between help seeking, and knowledge of depression. However, these studies did not utilize reliable instruments with evidence for validity, to measure the relationship between knowledge seeking and clinical improvement, which I aimed at in the current study. In the current study, the KSI, was utilized to examine the extent of seeking depression knowledge by patients, in a systematic fashion. It was, reported that 55% of subjects who fulfilled the research diagnostic criteria of major depression did not seek help. The non-help seekers did not consider the episode serious, or could not recognize it at as an illness, and believed that they could handle the episode themselves. On the other hand those who sought help, felt that the episode was too painful, lasted too long and caused disruption of their interpersonal, and role functioning [2]. The relationship between depression literacy per se and behavior change such as help seeking among patients was examined in a number of studies, which supports the evidence that patients' knowledge and attitudes towards depression, and its treatment influence the choice of treatment modalities especially antidepressants medication and play a role in stigmatizing people with depression [29] [30] [31]. For example, in one large study (n = 2010), respondents who had poor knowledge as shown in recognizing health problems in a vignette were less likely to recommend treatment from a counselor, psychologist or a psychiatrist, and some considered psychiatrists as harmful [29]. In the present study, although patients in the waiting group did not follow a systematic depression education, their educational activities and their symptoms were monitored and were measured systematically by the same instruments and at the same intervals as this was measured in the intervention group. In this manner, researchers were be able to compare the changes in symptoms associated with systematic education with those associated with no-systematic education as this might takes place in real life situation. It was demonstrated in literature that despite increased professional contact by those with major depression and suicidal ideation, there were few differences among three groups (depression with suicidal behavior, depression without suicidal behavior, and a control group) on either open-ended or direct questions related to mental-health literacy. This suggests that increased professional contact in itself was not related to increased mental-health literacy and that more specific psychoeducational programs are required [2]. This supports the findings in the present study that the number of visits to the psychiatrist did not seem to have statistically significant impact on depressive symptomatology scores, or the mean scores of knowledge seeking, as did the exposure to the systematic education over time. However, these results need to be examined in larger studies. Limitations of Psychoeducational Programs in Depression | ||||||
|
Conclusion
| ||||||
|
Systematic patient education about depression utilizing multimodal methods including reading material, audiovisual resources, and internet surfing was found to be associated with significant reduction in clinical symptomatology. In the current study, there is evidence to support that patients who sought more knowledge were more likely to present less depressive symptomatology over time. However, it is less clear if such positive clinical outcomes such as reduction in the severity of symptoms are closely related to seeking knowledge of depression. | ||||||
|
Acknowledgements
| ||||||
|
I would like to extend sincere thanks to all medical staff who participated in this study. My special thanks to Ms Marilyn Farmer, who delivered sessions of patients education, and to Zahra Ali, Moheb Basta, Mona Nematian, and Andrew Anderawis, for their assistance in data entry. | ||||||
|
References
| ||||||
| ||||||
|
[HTML Abstract]
[PDF Full Text]
|
|
Author Contributions:
Adel Gabriel – Substantial contributions to conception and design, Acquisition of data, Analysis and interpretation of data, Drafting the article, Revising it critically for important intellectual content, Final approval of the version to be published |
|
Guarantor of submission
The corresponding author is the guarantor of submission. |
|
Source of support
None |
|
Conflict of interest
Authors declare no conflict of interest. |
|
Copyright
© 2015 Adel Gabriel. This article is distributed under the terms of Creative Commons Attribution License which permits unrestricted use, distribution and reproduction in any medium provided the original author(s) and original publisher are properly credited. Please see the copyright policy on the journal website for more information. |
|
|
|
About The Author
| |||
| |||